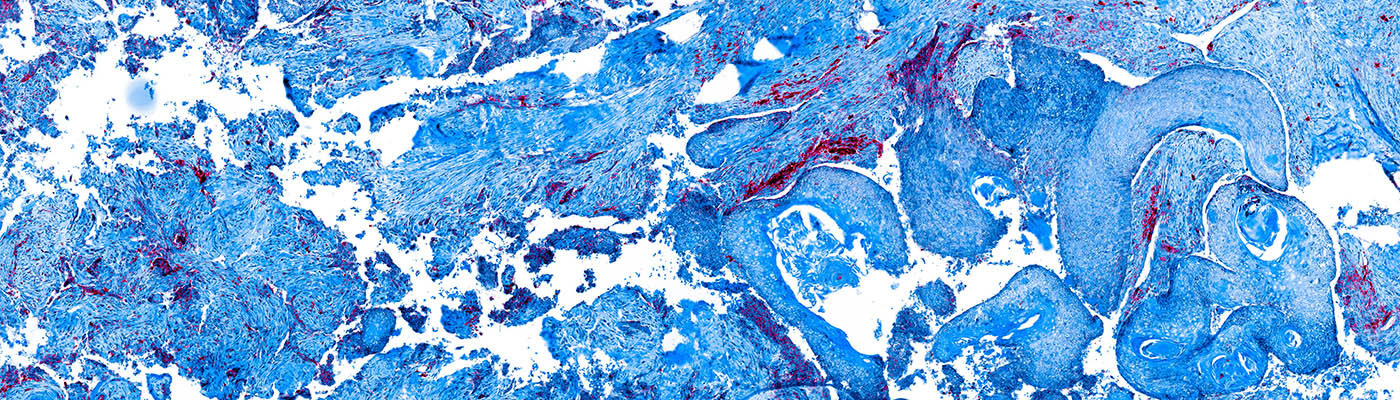
Brain tumours
Brain tumours can be benign (non-cancerous) or malignant (cancerous). While benign tumours can often be cured with surgery, the required brain surgery has the risk of neurological harm including stroke and loss of important senses like hearing and sight.
In some, the damage caused by surgery would be too severe and therefore they cannot be completely removed. Other treatments such as radiotherapy then become important, although they have their own side effects.
Improving research into brain tumours
Benign brain tumours receive very little funding because they are not cancer, but they have a massive impact on the quality of patients’ lives. These tumours include the most common primary brain tumour called meningioma, as well as other tumours such as vestibular schwannoma and pituitary neuroendocrine tumours.
At the other end of the spectrum, brain tumours are the biggest cancer killer of children and adults under 40. Around 12,000 people are diagnosed each year with a primary brain tumour – equivalent to 33 people every day.
They have been described as a cancer of ‘unmet need’, reflecting their disproportionate socioeconomic impact and in particular the failure to achieve comparable improvements in outcomes, to those seen in other cancer types.
A 2018 Department of Health report on brain tumour research highlighted that despite accounting for only 3% of cancers in the UK, brain tumours account for more deaths in men aged under 45 than prostate cancer, and more than breast cancer in women under 35.
We want life expectancy for even the most aggressive tumours to be better, but there has been very limited improvement for the past 6 decades. Research offers the only real hope of dramatic improvements in the management and treatment of brain tumours.
In Manchester, we treat the most brain tumour patients in the UK, and we are the only centre to be able to offer all modalities of treatment, including proton beam therapy.
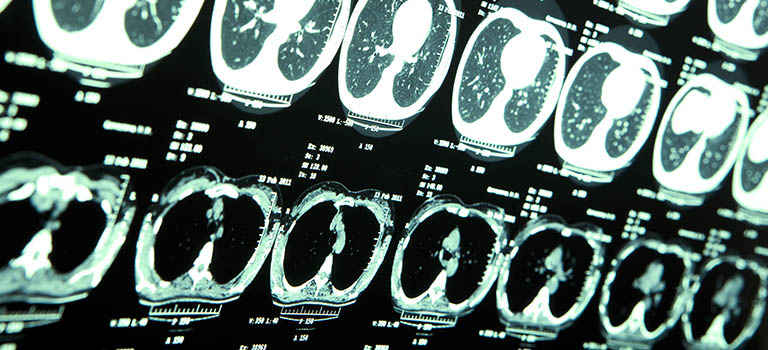
Neurofibromatosis type 1 and 2
Brain tumours can also be part of a genetic (inheritable condition). Two of the more common (but still rare) conditions are NF1 and NF2.
Although the names are very similar, they are very different and produce entirely different sorts of brain tumours.
Neurofibromatosis tumours are related to mutations in genes that play key roles in suppressing cell growth in the nervous system. These mutations keep the genes NF1 and NF2 from making normal proteins that control cell production.
Manchester is one of two NF1 specialist centres in England. For NF2, it is the lead centre for the NF2 service. Globally, five of the top NF2 25 experts in the world are in Manchester.
The world-leading NF2 research in Manchester has led to investment from the international charity NF2 BioSolutions, which has funded the Geoffrey Jefferson Brain Research Centre to host two PhD students. Read more on the NF2 BioSolutions blog.
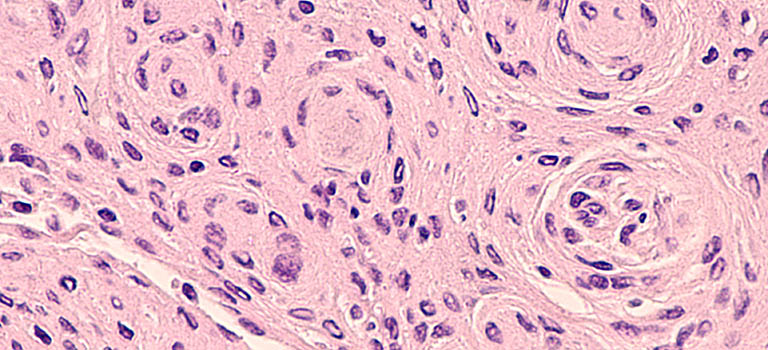
Our research
To demonstrably improve survival and quality of life in patients with brain and skull base tumours, we need to discover better treatments and rapidly translate basic science findings into healthcare benefit.
We aim to do this by:
- developing a leading centre for clinical and pre-clinical trials;
- establishing a Phase 0 study centre;
- developing a leading centre for radiobiology and quality of life;
- leading a multicentre Phase III study from our candidate agents targeted at the inflammatory microenvironment.
Research projects
Molecular profiling of gliomas using tear fluid
Funder: Brain Research UK
Local researchers: Professor Petra Hamerlik, Professor Marloes Peeters, Professor Alex Casson Clinical researchers: Dr David Coope and Professor Maria Castro
Researchers are working on a new way to detect brain tumours using tear fluid. This could help doctors diagnose brain tumours earlier and more accurately, leading to better, personalised treatments.
Low-grade gliomas are slow-growing brain tumours that mostly affect teenagers and young adults. Current treatments include surgery, radiotherapy, and regular MRI scans. Unfortunately, these tumours often progress to a more aggressive form, with a poor prognosis of about two years. Some of these tumours have specific gene mutations (IDH) that can help predict how well a patient will respond to treatment. Detecting these mutations early can help doctors choose the best treatment.
Currently, detecting these mutations requires invasive procedures like biopsies or collecting cerebrospinal fluid, which can be risky. Blood tests for cancer markers exist but don’t work well for brain tumours because the brain doesn’t release these markers into the blood.
Researchers are developing a device to detect a substance called D-2HG in tears, which is produced by tumours with the IDH mutation. This approach is based on promising early data.
This non-invasive device could make diagnosing brain tumours easier and more precise. It could help doctors understand the prognosis better and choose the best treatment earlier, improving patient outcomes and advancing personalised medicine.
Researchers are working closely with clinical colleagues to ensure the research can be quickly applied in clinical settings.
Interleukin-1 in Vestibular Schwannoma (IL-VS): A biomarker development study
Funder: Confidence for Translation (C4T) award.
Clinical researchers: Professor Andrew King, Dr David Coope, Professor Omar Pathmanaban, Dr James Galea, Dr Daniel Lewis
Academic researchers: Professors David Brough and Kevin Couper
In vestibular schwannoma (VS), inflammation is associated with tumour growth and studies have shown that one chemical mediator of inflammation called interleukin-1 (IL-1) is increased in patients with growing VS. Targeting IL-1 through drugs such as Anakinra (Kineret ©) could reduce inflammation and growth in these tumours. The first step and this study aim though is to understand the best tests or biomarkers that can evaluate whether targeting Il-1 is having an effect within VS.
For this study, ten patients due to undergo surgery for a growing sporadic or NF2-related Schwannomatosis VS at Salford Royal Hospital will be recruited. Participants will first undergo a research MRI scan for evaluation of tumour imaging biomarkers. Blood samples will also be collected so that levels of circulating pro-inflammatory chemicals (cytokines) can be evaluated. Following these tests, participants will receive a once-daily subcutaneous dose of an established, safe IL-1 targeting drug called Anakinra (Kineret ©). This drug will be given for 14 days at home by a trained member of the research team, and at the end participants will then undergo the same MRI scan and blood tests described above so that changes can be measured. During planned surgery, excess tissue from the tumour (VS) will be taken and specialised tests used to look for changes in the expression of inflammation related genes and changes in the number of inflammatory cells. To better understand how well these imaging, blood and tissue tests can detect the effects of IL-1 targeting, a separate group of 10 patients with growing sporadic VS listed who are due to undergo surgery will also be enrolled. This group of patients will not receive anakinra but will undergo the same tests detailed above, with MRI imaging and blood collection at day 0 and day 14, and analysis of resected tumour tissue.
USPIO enhanced MR Imaging in CNS tumours (UMIC) study
Current Funders:
Dowager Countess Eleanor Peel Trust
EANS research fund
MRC DTP studentship scheme
Clinical researchers: Dr David Coope (Chief investigator), Dr Daniel Lewis , Prof Andrew King
The immune response or inflammation is known to be a key driver of progression and growth in many solid tumours. Inflammatory cells called macrophages are present in high numbers in many brain tumours and these tumour associated macrophages or TAM are thought to have prognosis and treatment implications in these tumours. A key question, however, is how this inflammation or TAM abundance can be detected, measured and monitored in the clinic.
A clinically applicable imaging test that can directly and accurately measure tumour macrophage content would be of considerable value and one technique that may provide this is USPIO enhanced magnetic resonance imaging (MRI). Following intravenous injection, USPIO or ultrasmall superparamagnetic iron oxide nanoparticles, circulate in the bloodstream before being taken up by inflammatory cells/macrophages in tumour tissue, wherein they can be detected by MRI. This pilot study is to evaluate if a commercially available USPIO preparation called ferumoxytol (Feraheme ©) can accurately quantify macrophage abundance in brain tumours, with an exploratory focus on sporadic and NF2-SWN associated vestibular schwannoma (VS) and suspected transforming low-grade glioma (LGG). Patients with both non-growing (static) and growing VS, and patients with suspected transforming LGG will undergo dedicated MRI sequences before, immediately after (< 2 hours) and at both 24 and 48hrs after ferumoxytol administration. In patients undergoing surgery, acquired imaging will be compared with resected tumour tissue so that markers of inflammation can be compared with USPIO uptake. Through advanced laboratory methods this study will seek to establish within resected VS and LGG specimens: the cellular destination/s of USPIO uptake; the nature of the inflammatory and/or tumour cells containing the USPIO; and the relationship between USPIO uptake and tumour blood vessel permeability or leakiness.
Characterising the immune microenvironment of chordoma
Current Funders:
Dowager Countess Eleanor Peel Trust (DCEPT)
Clinical researchers: Dr Inga Usher, Prof Omar Pathmanaban
Chordomas are rare bone cancers that develop at the base of the skull and in the spine. Surgery and high dose radiotherapy are the only treatment options but both are associated with side effects that can hinder quality of life. As genetic mutations are relatively rare in chordoma, we are studying the immune cells in a large number of chordomas to see if we can identify subsets of chordomas that could be treated differently. This has not previously been performed on a large scale. Studying the immune cells in other cancers has improved their treatment. By using different technologies including methylation profiling, RNA sequencing and single cell RNA sequencing we hope to achieve this for chordomas.
Basic science research
SNOMan Lab
The Surgical Neuro-Oncology Manchester lab investigates the biology of and treatments for brain and skull base tumours.
- Twitter: @SNOMAN_Lab
Investigators
 David Coope
David Coope
 Catherine McBain
Catherine McBain
 Petra Hamerlik
Petra Hamerlik Gerben Borst
Gerben Borst Omar Pathmanaban
Omar Pathmanaban Tom Kisby
Tom Kisby  Martin McCabe
Martin McCabe Andrew King
Andrew King Gareth Evans
Gareth Evans