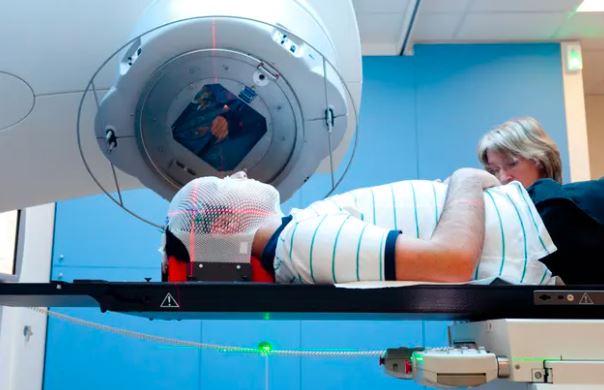
Pioneering study targets brain tumours with radiotherapy before surgery
A patient has had pioneering pre-surgery treatment as part of a new clinical trial for people newly diagnosed with a brain tumour.
Joel Rush, 45, from Denton in Greater Manchester is taking part in a study, known as POBIG (Pre-Operative Brian Irradiation in Glioblastoma), which is trialling radiotherapy before brain surgery, on what could potentially be a game-changer for the treatment of the most common type of brain tumour. His treatment involved radiotherapy at The Christie NHS Foundation Trust before surgery at Salford Royal, part of Northern Care Alliance NHS Foundation Trust.
By giving highly targeted radiotherapy before surgery, the aim is to try to stop the tumour from growing back so quickly to improve outcomes and extend lives.
Treatment for glioblastoma usually involves an operation, followed by radiotherapy, and then chemotherapy. Even with this intensive treatment, less than 10% of people live for five years or more. Glioblastoma is one of the most difficult types of cancer to treat, the fastest growing and the one giving patients the poorest prognosis.
Despite extensive research involving hundreds of clinical trials, there is no cure, and the standard sequence of surgery followed by post-operative treatment has never been challenged.
Better strategies
Dr Gerben Borst, radiation oncologist at The Christie NHS Foundation Trust and senior lecturer at The University of Manchester, who is leading the study said: “It’s essential patients with brain tumours have surgery. However, surgery cannot remove the whole tumour, and the procedure can aggravate the remains. In other words, remnant tumour cells remain growing, potentially even more aggressively, post-surgery in the recovery period before the patient is given the standard course of radiotherapy. Therefore, better strategies are desperately needed to target all tumour cells at an earlier stage. As a tumour is likely to respond better to radiotherapy before the operation, we hope, by giving highly targeted radiotherapy before surgery, to stop the tumour from growing back so quickly to improve outcomes and extend lives.
 Dr Borst (pictured), who is also a theme lead for brain tumours at The Geoffrey Jefferson Brain Research Centre added: “This study is an important and significant milestone in brain cancer research, and the culmination of 10 years’ work for me. The order of radiotherapy and surgery should be challenged, and this could be the breakthrough we have been working towards for decades. Progress in treating brain tumours has not happened for several reasons – such as drugs not reaching the brain tumour because of its protective barrier, the fact glioblastomas can be very different, and neurosurgeons can’t remove all the tumour because of the damage it would cause. Although research has led to a better understanding of tumour characteristics, this hasn’t translated into the cure or personalised treatment of glioblastoma patients. For patients who are not in a medical emergency and need to undergo immediate surgery, we know that the outcomes are not affected as long as surgery is done within a couple of weeks. This allows us to apply a treatment that targets all the tumour cells that are inevitably left behind after the surgery at an earlier stage. I really hope that our study motivates and encourages others to join our efforts in seeking more effective and personalised treatment strategies to be applied before surgery.
Dr Borst (pictured), who is also a theme lead for brain tumours at The Geoffrey Jefferson Brain Research Centre added: “This study is an important and significant milestone in brain cancer research, and the culmination of 10 years’ work for me. The order of radiotherapy and surgery should be challenged, and this could be the breakthrough we have been working towards for decades. Progress in treating brain tumours has not happened for several reasons – such as drugs not reaching the brain tumour because of its protective barrier, the fact glioblastomas can be very different, and neurosurgeons can’t remove all the tumour because of the damage it would cause. Although research has led to a better understanding of tumour characteristics, this hasn’t translated into the cure or personalised treatment of glioblastoma patients. For patients who are not in a medical emergency and need to undergo immediate surgery, we know that the outcomes are not affected as long as surgery is done within a couple of weeks. This allows us to apply a treatment that targets all the tumour cells that are inevitably left behind after the surgery at an earlier stage. I really hope that our study motivates and encourages others to join our efforts in seeking more effective and personalised treatment strategies to be applied before surgery.
“The POBIG study is a team effort, working alongside neurosurgeons, oncologists, nurses, radiologists, physicists, and pathologists, and importantly patient support groups like the Brainstrust. Besides the novelty of irradiating the tumour before surgery, other innovative aspects are that we base the diagnosis on imaging so as not to delay the treatment. Crucially we don’t irradiate the whole tumour, only the part where the neurosurgeon believes the remnants will be left behind. This prevents interference with the standard clinical pathway of looking into specific tumour characteristics and offers unique opportunities to develop more personalised treatment strategies against this life-limiting disease. We are very pleased with how Joel has responded to this treatment and the result so far is very encouraging. We are hopeful this technique could improve outcomes for all patients like Joel in the future.”
Treatment options
Mr Pietro D’Urso, speaking on behalf of the Neurosurgical Oncology team at Salford Royal where the surgery took place, said: “There are very limited treatment options for this form of brain cancer, and this trial will look into the potential benefits of pre-operative radiotherapy in improving patients’ outcomes. This trial also constitutes a unique research opportunity.
“We are privileged to work with our colleagues at The Christie and honoured to be supporting Dr Gerben Borst, and our colleagues at The Christie.
“Team-work results in better care for our patients as well as enabling us to deliver innovative treatments and we are grateful to all people involved into this trial, including our Neuroradiology and Neuropathology Colleagues.”
Adding to knowledge
Joel Rush, a previously fit and healthy married father of two, first noticed a problem in August 2022 when he had suddenly lost concentration like he was daydreaming while mountain-biking, causing him to crash. Two weeks later he started to experience numbness down the whole of his left side and went to A&E. Subsequent CT and MRI scans were not indicative of a brain tumour and Joel was treated for a stroke. In October he started suffering prolonged headaches for two weeks, and then one day woke up with severe pain in his head, unlike anything he’d experienced before. The scans were repeated and this time revealed a completely different picture. A tumour the size of an egg was seen and he was given the devasting diagnosis he had a glioblastoma, an aggressive and incurable type of brain cancer.
In November, Joel, a director of a digital marketing agency who he co-founded with his wife Tracey, was offered the chance to participate in the POBIG phase 1 (early phase) study. This meant that two days before his operation, a high dose of radiotherapy was administered to the parts of his tumour that couldn’t be removed during surgery.
Joel said: “Being initially treated for a stroke meant they couldn’t operate straight away due to the blood thinning drugs. That gave the medics time to get me on the POBIG trial. The doctors explained the reasons for using radiotherapy before surgery, made absolute sense, so I was very happy to participate in the trial. I love learning, so if I can help others like Dr Borst and his team gain knowledge which can help others like me, that can only be a good thing. It’s still early days but I hope this early intervention will benefit me in the long term.”
Neurosurgical excellence
The study, which is currently only taking place in Manchester, aims to recruit 18 patients in total. The surgery takes place at Salford Royal, part of Northern Care Alliance NHS Foundation Trust, which is a centre of excellence for neurosurgery. This new approach, is being piloted by oncologists based at The Christie, working closely with brain surgeons (neurosurgeons), brain imaging specialists (neuroradiologists) and pathologists for the nervous system (neuropathologists) based at Salford Royal. The innovative treatment on the POBIG trial is only suitable for newly diagnosed patients whose scans indicate they have glioblastoma and not in a medical emergency to undergo immediate surgery. Patients with glioblastoma typically survive for under six months if left untreated.
Any patients interested in taking part in clinical trials should be referred through their consultant or GP.
POBIG and its translational scientific programme is supported by Medical Research Council UKRI, Cancer Research UK RadNet Manchester and the Manchester Cancer Research Centre. The Christie is the study’s sponsor.
The Brain Tumour Charity and the Brainstrust helped with the study design.
Article by Claire Mooney, Research and Innovation Communications Manager, Northern Care Alliance NHS Foundation Trust



0 Comments